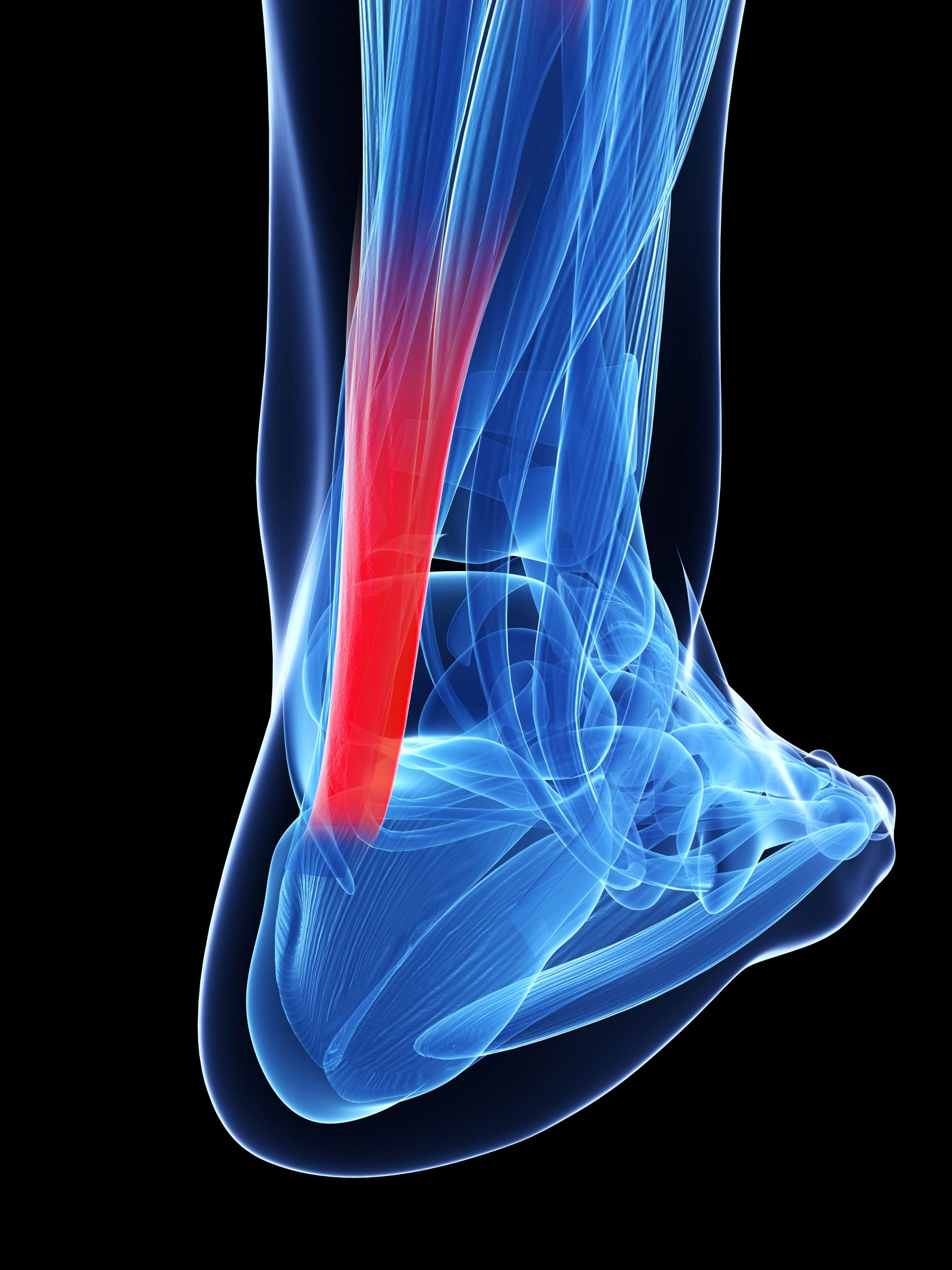
Achilles Injury: A Comprehensive Guide
The Achilles tendon joins your calf muscle to the heel bone (calcaneum). It acts with the calf when you push up onto your toes. This action becomes more forceful when you push off to start to sprint. It is at this time when the tendon may be injured due to the high levels of force placed through it. This also applies with jumping, pivoting and sidestepping.
The Injury
 The most common type of Achilles pain is from a tendinopathy. This is where the tendon becomes thickened and sore. It is often sore first thing in the morning when you get up to walk or when you get up from sitting. It usually eases off with movement but then becomes sore again if you do too much activity.
The most common type of Achilles pain is from a tendinopathy. This is where the tendon becomes thickened and sore. It is often sore first thing in the morning when you get up to walk or when you get up from sitting. It usually eases off with movement but then becomes sore again if you do too much activity.
If you experienced a sharp Achilles pain during a sporting activity it is possible to either partially or fully tear your Achilles tendon. If you heard a pop/snap and felt like you were hit in the back of the leg by something then you may have a full tear. If this is the case you may have experienced a sharp pain at the Achilles at the time of the incident, which subsided to a dull ache or even no pain at all afterwards. You will struggle to walk on that side, will find it hard to go up stairs and may be unable to push up onto your toes.
Treatment
Tendinopathy
If your Achilles is just a bit sore then it is likely to be a tendinopathy. This is managed through physiotherapy. Tendons do not have a very good blood supply and so do not simply heal well on their own with time and rest. Research shows that tendons need to be put under a gradually increasing loading protocol to help them to heal. There are differing levels of exercise to do this and it is our job as physiotherapists to determine the appropriate loading strategy for your Achilles. We would rehabilitate you to the level that you require for your day to day activities and hobbies. This may simply be to walk again pain free, or it may involve high level plyometric exercises for a full return to sport.

Partial or Full Thickness Tear
It is vital to have your injury assessed. If you think you may have ruptured your Achilles tendon then you should go to A&E immediately. A test that they may perform is the ‘squeeze test’ where you lie on your front and they squeeze your calf muscle. If the tendon is intact your foot will move. If it is ruptured the foot will stay still when they squeeze your calf.
Non-Surgical (Conservative) Treatment
Depending on your age and activity level the Achilles injury may be treated conservatively by placing your lower leg in a cast. This will be for 6-8 weeks and it will be taken off and changed a few times over this period so that they can alter the angle of your ankle as the tendon heals. Once the cast is no longer required you will start a graded physio rehabilitation program. This is a vital stage in the healing process as you gradually expose the tendon to higher forces. You would progress through a range of exercises to build strength in the calf and Achilles tendon, meanwhile maximising mobility in the ankle and ensuring good strength in the leg as a whole.
Surgical Treatment
The ruptured tendon will be repaired surgically and your lower leg will then be placed in a cast or brace for 4-6 weeks. Once removed you will start a graded rehabilitation program. It is critical to work hard at these exercises to lower your chance of re-rupturing the tendon at a later date. Higher level activity can generally begin at roughly 4 months but it may take up to a year for an athlete to return to the level of activity they were at prior to the injury. It is a long process but you should fully recover and be able to take part in all forms of sport again.
Whether you have had conservative or surgical management we would test you on our force plates which show in incredible detail how the leg is functioning compared to the uninjured side. We can use this information to judge how to progress your rehab and also determine when you are ready to return to activities/sports.

Prevention of an Achilles Injury
There is no research to show that stretching prior to exercise helps to avoid injury. It is more important to warm up well. The main prevention is to ensure that your calf is strong and flexible. Your gym training should include calf raises and plyometric exercises (bounding/jumping). This regular stress placed on the Achilles causes it to improve it’s tolerance to mechanical stress, making it less likely to be injured when you do something that challenges it. If you are starting your fitness journey, perhaps embarking on a running program to build up to a 10km, half marathon or even a full marathon, you should be thinking about how you can improve your tissue capacity so that it can tolerate this increased use. We see too many people in clinic who have become sore as they build up their volume of running. The problem occurring when they are running longer distances, which are inevitably close to the event. At this point we can still help but it would have been much better to start some preventative work at the beginning of your fitness journey. There is lots of scientific evidence to show that this is the best strategy and is very effective at minimising the risk of injury. Get in touch if you have any questions and would like to discuss this approach.