Explore comprehensive treatments for women’s health through specialised physiotherapy care.
WOMEN’S HEALTH
Overview
Available at: PRESTONFIELD
There are many reasons seeing a Women’s health specialist physiotherapist may be helpful. We can help at many different stages in life, whether it is ante or postnatal, peri or post-menopausal and everything in between. A lot of the time women are embarrassed to talk about their pelvic floor problems or think it is a normal part of ageing or having a baby, it’s not, and we can help!
If you are struggling with pelvic pain, urinary incontinence, overactive bladder, faecal incontinence, constipation, painful intercourse or would just like advice on how to get back to exercise or normal activities after a baby or surgery we can help. Pelvic floor physiotherapy is a recommended treatment in NICE (National Institute for Health and Care Excellence) guidelines on pelvic floor dysfunction, prolapse and urinary incontinence.
Women’s health physiotherapists have completed specific post graduate training in pelvic floor assessment and are able to take a holistic approach to your rehabilitation to help you achieve your goals through exercise, lifestyle advice and manual treatment if needed.
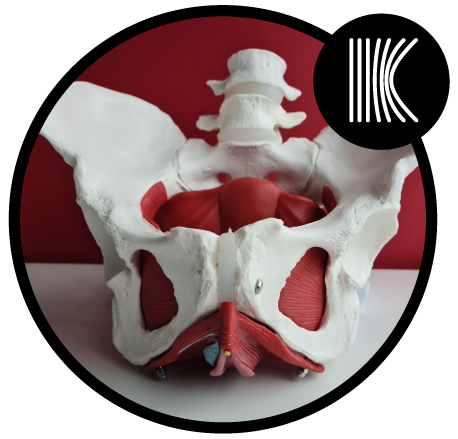
Pelvic floor dysfunction and Women’s Health physiotherapy
Available at: PRESTONFIELD
Your pelvic floor muscles are part of your deep core and sit like a hammock at the base of your pelvis. The role of your pelvic floor muscles is to maintain continence of urine, flatulance and faeces, support the pelvic organs and pelvis and they have a role in sexual function.
The pelvic floor muscles need to be strong enough to support the pelvic organs and maintain continence even under high loads such as running, carrying shopping or children or just sneezing. The pelvic floor muscles also need to be able to relax to allow intercourse, examinations such as a smear test or tampon or moon cup use and defecation.
Your bladders job is to store urine until a suitable time. Sometimes the bladder can become overactive, causing symptoms such as increased frequency of urination, nocturia (getting up more than once overnight), urgency (not getting much warning of needing the toilet) and urge urinary incontinence (leaking before you get to the toilet).

Antenatal Physiotherapy
Available at: PRESTONFIELD
Growing a baby is hard work! The growing baby sitting on your pelvic floor and hormone changes can cause pelvic floor dysfunction such as stress incontinence.
Low back, pelvic and hip pain can all be common complaints during pregnancy as your body changes and adapts.
Pelvic girdle pain (PGP) describes pain felt around the pelvis, commonly over the pubic bone which sits in-between your legs. Changes in biomechanics, hormone levels and load on the pelvis can contribute to this pain but we now know through recent research that an increase in sensitivity of the nervous system (the brain, spinal cord and nerves) contributes hugely to PGP.

Postnatal Physiotherapy
Available at: PRESTONFIELD
Having a baby is a wonderful, exciting and terrifying time! Understandably your new baby gets a lot of the attention but what about you? You may have specific concerns around an obstetric trauma to your pelvic floor or caesarean section scar. You may be left with a lot of questions about your recovery and how to safely return to your normal activities or sport. We can help guide your recovery and get you to feel more like yourself.

Menopause
Available at: PRESTONFIELD
Going through the menopause can cause a huge range of symptoms, some we are familiar with such as hot flushes, mood changes and anxiety. There are also a lot of changes occurring within the pelvis as hormone levels fluctuate and decrease. There are oestrogen receptors throughout the female body, which is why menopause symptoms can be so varied. These are most concentrated in the pelvis. The muscles, ligaments, connective tissue, bladder, urethra and bowel all go through changes during and after the menopause due to the lower level of hormones. This can lead to problems such as incontinence, prolapse, vaginal dryness and painful intercourse. These complaints should not be accepted as part of the normal ageing process. Women’s health physiotherapy can help with all these symptoms.

What happens at Women’s Health Physiotherapy appointment?
Available at: PRESTONFIELD
You will be assessed by a highly qualified female physiotherapist in a private room. We will take a detailed history of your problem and general lifestyle. When it is appropriate you will be offered a physical examination. The nature of the examination depends on why you are coming. It may, with your consent, involve an internal examination, either vaginally or rectally. This will be fully discussed with you, you do not have to have an internal examination if you are not comfortable with this. You are welcome to bring a chaperone to the appointment if that makes you feel more comfortable.
Physical assessment may include:
- Assessment of your posture
- Joint range of movement and control
- Core muscle control of your abdomen
- Diastais Recti (separation of tummy muscles) is very common postnatally, early assessment can ensure you are doing the correct exercises to aid your recovery
- Internal examination of the pelvic floor, to ensure it is contracting and relaxing correctly. Problems in the strength of the pelvic floor or its ability to relax can affect continence, intercourse and its support of the pelvic organs. Having a strong healthy pelvic floor is crucial in returning to higher impact exercise and to prevent any future problems.
- Review of a bladder / fluid diary
Following assessment treatment options may include:
- Tailored pelvic floor exercise program, with a clear plan for progression
- Pilates based exercises to assist in recovering core strength of the abdominals and pelvic floor
- Down training of the pelvic floor muscles
- Relaxation and breathing exercises
- Fluids advice and advice on positioning for passing urine and stools
- Return to running and higher-level exercise plan
- Caesarean section, obstetric tear and episiotomy scar management through manual treatment and advice
- Internal manual therapy treatment to aid relaxation of the pelvic floor
- Soft tissue release treatment of the pelvic floor, abdominal or pelvic muscles
- Advice on pelvic floor muscle stimulators, educators and vaginal weights to improve your strength and awareness of your pelvic floor muscles
- Advice on medication which can help with bladder and bowel function
- Advice on supportive garments and vaginal devices for stress urinary incontinence
- Pain education
- Bladder retraining

Get in touch
Please don’t hesitate to get in touch with Olivia if you have any questions which you would like to discuss before booking an appointment: olivia@kineticphysio.co.uk









